Category Myths & Misconceptions

Why does our local CAP guideline differ from Australian Therapeutic Guidelines?
Kristi, Lorrae and Ayesha have recently joined as AIMED authors– welcome aboard. Here’s a posting from Kristi that unpacks the approach to community-acquired pneumonia (CAP) in Hunter New England Health, NSW. In adults, the most common bacterial cause of community-acquired pneumonia (CAP) is Streptococcus pneumoniae. Other pathogens associated with CAP include Haemophilus influenzae and atypical’ […]

“UTI” – Requiem for a Heavyweight – a landmark paper
A recent paper, “Urinary Tract Infection”-Requiem for a Heavyweight by Dr Thomas Finucaine skillfully unpacks many key issues, coupling this with a consideration of the emerging knowledge of the urinary microbiome and virome, suggesting that the term “UTI” might better be referred to as a “urinary dysbiosis”. The paper is worth a detailed read – here […]
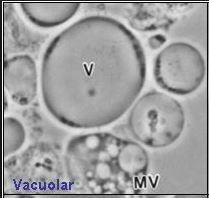
Blastocystis- commensal or culprit? Do I really care?
Guest posting from Dr Hema Varadhan, Clinical Microbiologist, Pathology North. This parasite intrigues me every time I validate a faecal PCR result. Why do we see these bugs more often than the others? Do we care? Do we need to treat? The RCPA recently provided relevant guidance concerning Blastocystis and Dientamoeba which is also useful […]

Penicillin ‘allergy’ and safety of third generation cephalosporins (ceftriaxone)
A frequent issue is deciding whether a patient with a “penicillin allergy” can safely be given a cephalosporin antibiotic – what is the real risk of cross reaction and is it much less for third generation agents such as ceftriaxone? A recent publication in Prescriber Update from Medsafe New Zealand succinctly analyses cross-reactivity amongst beta-lactam antibiotics in the light […]
Wasted spectrum 101 – amoxicillin+clavulanate overuse
Amoxicillin+clavulanate (Augmentin) is an important broad spectrum agent that includes Gram negative anaerobic coverage (see below). We rely on it for a variety of complex infections, often as a second line. Compared with amoxycillin alone, the incidence of gastrointestinal, hepatic and haematological side effects is significantly higher for amoxicillin+clavulanic acid. It may be associated with a […]

Treatment of boils – Oz GPs reluctant to rely on scalpelmycin rather than antibiotics
Are you following best practice in the management of boils or recurrent skin infection? We’ve previously addressed this matter detailing a NEJM study that indicated that a majority of US doctors surveyed use incision and drainage only. This recent Australian study investigated treatment of community staphylococcal skin abscesses by GPs and showed that a majority do not follow […]

Extrapolating antibiotic susceptibility for streptococci including the pneumococcus
This posting concerns betahaemolytic species of streptococci including S. pyogenes (Lancefield group A strep), S. agalactiae ((group B strep), S. dysgalactiae group (betahaemolytic large colony, groups C or G) (several species included) which are usually associated with pyogenic infection, especially of skin and soft tissue. S. pneumoniae (the pneumococcus ) is also considered. A key misunderstanding about […]

Cranberry for prevention and treatment of UTI- placebo or better?
Updated 25/1/24: Cochrane review was updated in Dec 2023 . “Authors’ conclusions: After a thorough search, no RCTs which assessed the effectiveness of cranberry juice for the treatment of UTIs were found. Therefore, at the present time, there is no good quality evidence to suggest that it is effective for the treatment of UTIs. ” Cranberry […]

Relative mortality risk from antibiotic use compared
Much time is spent discussing the development of antimicrobial resistance and changes to the microbiome but perhaps should we should also focus on the potential for patient mortality. Based on best current estimates, trimethoprim, macrolides and quinolones may be less safe than chloramphenicol in certain patient populations. A future posting will provide a practical approach to the […]
Magical thinking- do antibiotics improve chronic wound healing?
We’ve previously addressed this topic here. It’s certainly the case that chronic skin ulcers (leg or elsewhere) drive an enormous amount of antibiotic prescribing, perhaps because these ulcers are so hard to heal and a degree of therapeutic impatience occurs. The annual survey of chronic wounds last year in our health district indicated that 28% of inpatients […]