An article in The Medical Observer by Dr. Sergio Diez Alvarez of the University of Newcastle comments on alarming trends of antibiotic resistance, the current problems with antibiotic stewardship and potential strategies to improve on reducing resistance. Whilst Dr Alvarez’s article provides some excellent comments for reflection on antibiotic use in humans, it is his discussion regarding antibiotic use in agriculture and cross resistance that make this article an interesting read.
Medical professionals and allied health workers may forget agricultural contributions to antibiotic resistance. What is of potentially more interest is the conflicting evidence as to whether antibiotic use in agriculture is directly contributing to resistance in humans. Facts of note from the article and previous AIMED posts:
- Around 80% of all antibiotics used in the US are given to farm animals, meaning that only 20% are actually used to treat infections in people (see Antibiotic Facts and Figures).
- Chicken, pork and farmed fish receive antibiotics such as tetracyclines that are also used to treat infections in humans, and antibiotics like avoparcin that cause cross-resistance to similar antibiotics used in humans.
- In 2000, Denmark banned most antibiotic use in agriculture. Dr Alvarez lauds this success but notes that their studies have so far shown this has NOT had the intended benefit of reducing antibiotic resistance patterns in humans (see full report for details).

Figure 1. Antibiotic use in human therapeutics (red) vs. agricultural products (blue) in Denmark, 1990-2009
The Danes’ AMS effort is currently spearheaded by the Danish Integrated Antimicrobial Resistance Monitoring and Research Programme (DANMAP). Their latest report reveals some interesting trends, with most levels of resistance increasing for most pathogens (with the notable exceptions of K. pneumoniae in blood and urinary isolates – see below).
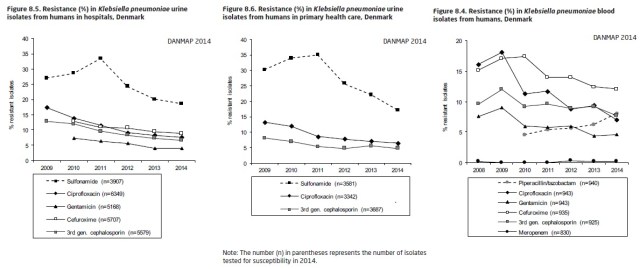
While it is fairly well accepted that antibiotic use in agriculture contributes to cross-resistance ( diagram from the CDC below), statistics like these (although representing associations only) lend an appreciation of the responsibility medical and health professionals have for judicious use of antibiotics. If the non-human sector is being more responsible in their use of antibiotics and human resistance levels are still growing, then the other primary user of antibiotics must be scrutinized more thoroughly!

References
- Danish Integrated Antimicrobial Resistance Monitoring and Research Programme. DANMAP 2014. Use of antimicrobial agents and occurrence of antimicrobial resistance in bacteria from food animals, foods and humans in Denmark.
-
Andremont, Antoine. “What to do about resistant bacteria in the food-chain?.” Bulletin of the World Health Organization. World Health Organization. April. (2015).
-
Centres for Disease Control and Prevention (US). Antibiotic resistance threats in the United States, 2013. Centres for Disease Control and Prevention, US Department of Health and Human Services, 2013.